Melasma vs Freckles, Sunspots, and Hyperpigmentati
Several conditions can result in changes in skin color, and a few of them even look similar to the […]

We offer in-office appointments for medical dermatology, pediatric dermatology, skin cancer detection and treatment, Mohs surgery, aesthetics, and allergy solutions.

Specialized care for skin diseases and conditions for patients of all ages, from infants to the elderly.

A full range of cosmetic and aesthetic services for men and women, tailored to meet your skin care needs.
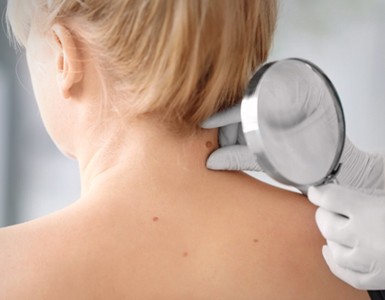
Get the facts on skin cancer symptoms, signs, treatment, and types (basal cell carcinoma, squamous cell carcinoma, melanoma).

Our allergy specialists offer several different options for allergy testing and solutions to help determine allergic reactions.
As scary as it is to see anyone in the healthcare field, especially for possible skin cancers, my experience was great. The PA Hannah was amazing and so kind when she was discussing my options. Her medical assistant Emely was very sweet as well. I would highly recommend going to their clinic for any of your skin care needs. Definitely five-star service!a long wait to get in for an appointment, which I appreciated since my schedule limits my free time. No one wants to go to the doctor but if I need a dermatologist again my first call will be to Affiliated Dermatology.
Morgan from the aesthetics office was so amazing. It was my first-time getting lip fillers and our consultation was so easy and she explained everything so I can understand and answered all my questions. I was so nervous and she assured me it would be fine. Even the day after and days after I was able to private message her with any concerns and she would reply quick with all my annoying questions and anxiety I had with the bruising. She had a lot of patience with me and I truly appreciate how caring and professional she is. I will continue to use this office for all my fillers! I strongly recommend her for all first-time fillers or for any service, she will make you feel taken care of and provide all details that will make your mind at ease.
I've needed to go to Affiliated Dermatology many times over the past 4 years. I've had several procedures to repair sun damage. They are always prompt, courteous, professional and friendly. I highly recommend them at every location and I've gone to several!

We are currently offering aesthetic appointments and complimentary consultations for select services …

Several conditions can result in changes in skin color, and a few of them even look similar to the […]
Everyone knows the importance of taking care of your skin. However, some people have more sensitive skin than others, […]

As a medical and surgical practice, Affiliated Dermatology® is open and committed to providing dermatological services. In order to safely accommodate our skin cancer and medical patients, we are taking the necessary precautions to maintain a safe environment at our practice.
A full-service dermatology group offering services in general dermatology, skin cancer detection and treatment, Mohs surgery, aesthetics, and allergy. At our Valley-wide locations, we take pride in our dedication to help inspire and empower you to make educated, healthy decisions about skin care.
Follow Us Online:
 Scroll Up
Scroll Up