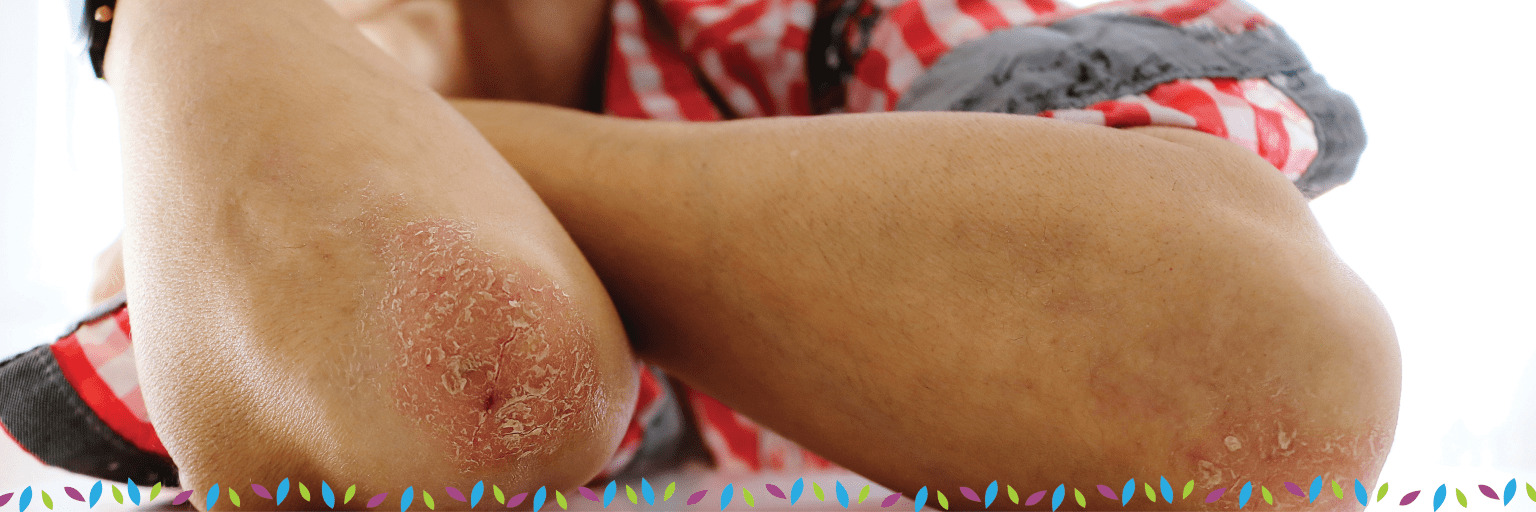
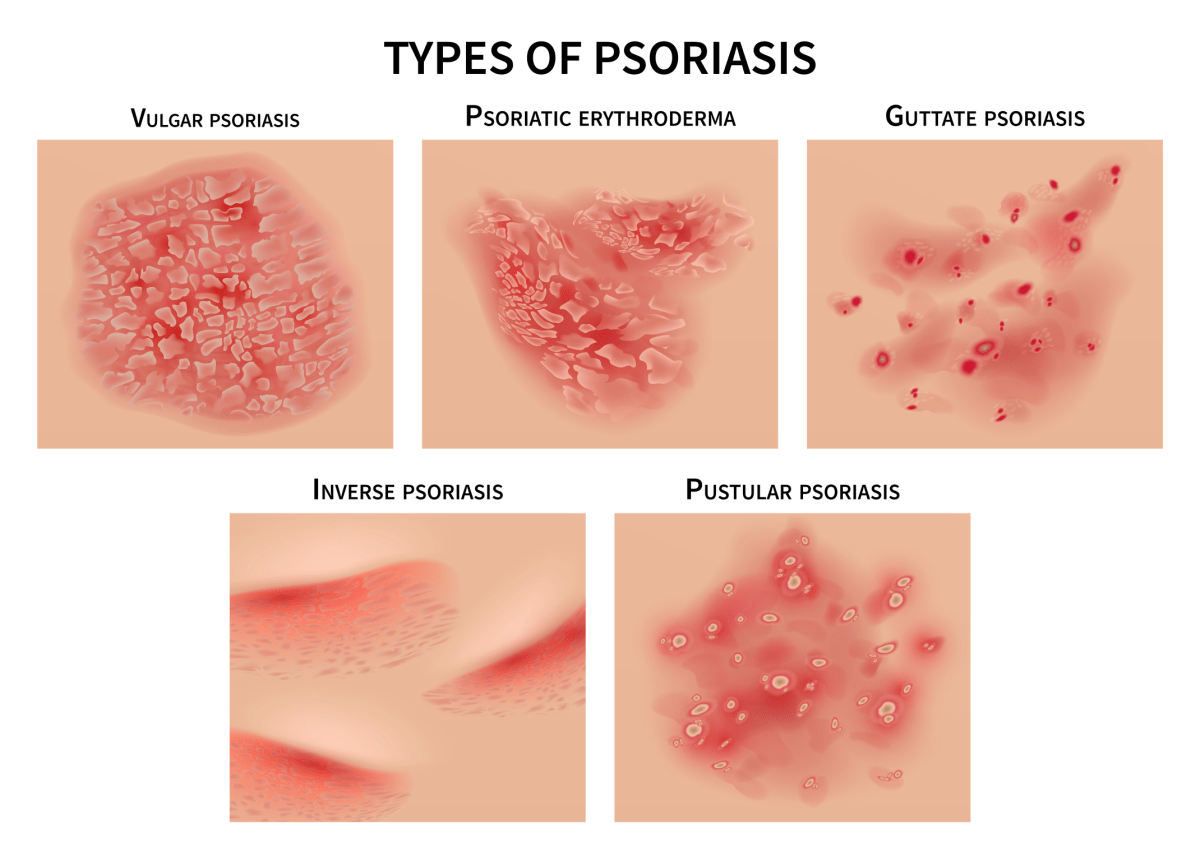
Psoriasis is a chronic skin disorder characterized by raised lesions with silvery scale that most often occur on the scalp, elbows, knees and lower back. It can range from a very mild, hardly noticeable rash to a severe eruption that covers large areas of the body. In some patients, psoriasis causes nail changes and joint pain (psoriatic arthritis).
Psoriasis affects 2% of people and is not contagious, but may be inherited. The first episode usually strikes between the ages of 15 and 35. It is a chronic condition that will then cycle through flare-ups and remissions throughout the rest of the patient’s life.
Light Therapy/Phototherapy: At Affiliated Dermatology, we are proud to offer cutting-edge Excimer Lamp Therapy, a transformative solution for both pediatric and adult patients suffering from psoriasis. The Excimer Lamp represents a leap forward in dermatological treatments. This sophisticated technology uses controlled ultraviolet light, targeting affected skin areas with precision. The result is a treatment that’s not only effective but also safe and minimally invasive.
Learn more about the EXCI30 laser with these FAQs provided by Aerolase.
Moderate-to-severe psoriasis treatments include prescription medications, biologics, and light therapy/phototherapy.
For more information or to schedule an appointment with a psoriasis specialist at one of our several dermatology offices in Arizona, please contact us by calling (480) 556-0446 or leaving us a message with the contact form below.
Whether you wish to receive treatment for a skin condition or an aesthetic procedure, you can be assured you will be treated with professional and personal care by one of our skin care experts. Please feel free to call us at (480) 556-0446 or leave us a message online using our Contact Us form.
A full-service dermatology group offering services in general dermatology, skin cancer detection and treatment, Mohs surgery, aesthetics, and allergy. At our Valley-wide locations, we take pride in our dedication to help inspire and empower you to make educated, healthy decisions about skin care.
Follow Us Online:
 Scroll Up
Scroll Up